PHLEBOLYMPHEDEMA
PHLEBOLYMPHEDEMA
Phlebolymphedema is a very common form of lymphedema. It is a condition created by a combination of chronic venous insufficiency and impaired function of the lymphatic system, that results in inflammation and lymphedema in the legs and feet.
Chronic venous insufficiency is a condition where the one-way valves in the veins in the legs that normally allow blood to flow only toward the heart, don’t close properly, and thereby allow the blood in the veins to flow backward toward the feet. This backward flow of blood causes more fluid to build up in the tissue spaces creating swelling, or edema, in the feet, ankles, and legs. The lymphatic system is made up of lymphatic vessels and lymph nodes that remove extra water from the tissue spaces to prevent edema from forming. In the early stages of chronic venous insufficiency, the lymphatic system may work efficiently to control the accumulation of extra water or edema in the tissues. At this stage, feet and ankles may be swollen at the end of the day, but the swelling reduces with elevating the legs overnight. However, as the venous insufficiency worsens over time, the extra fluid accumulating in the tissue spaces increases to the extent that the lymphatic system can’t keep up with removing it. As a result, the leg swelling becomes progressively worse and does not go down with elevation overnight. This swelling is called phlebolymphedema.
Causes of Chronic Venous Insufficiency.
There are many potential contributing factors to the development of chronic venous insufficiency. These factors include a family history of varicose veins, pregnancy, blood clots, leg trauma, and surgery on the legs. However, lifestyle factors such as being overweight, prolonged sitting or standing, lack of exercise, and smoking can also contribute to its development.
The Appearance of Chronic Venous Insufficiency.
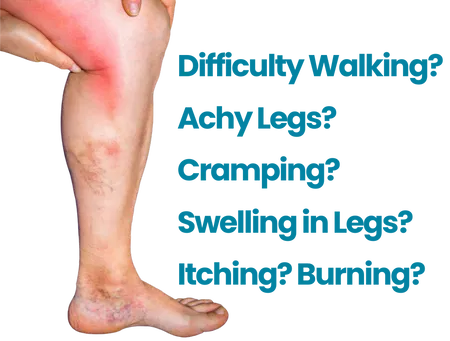
Chronic venous insufficiency can appear as a variety of color changes in the legs. These color changes include:
- Red and/or brown areas over the legs. This hyperpigmentation is called hemosiderin staining and is caused by the breakdown of red blood cells that have leaked out of the veins into the skin.
- Redness and heat in the legs are caused by inflammation.
- Purple varicose veins are enlarged and painful.
- Small, reddish-purple broken veins called telangiectasias or spider veins.
- Reddish-purple discoloration around the ankles accompanied by itching, thickened, skin (stasis dermatitis). In addition, as chronic venous insufficiency progresses, the skin becomes fragile and more susceptible to developing sores called venous stasis ulcers. These ulcers are slow to heal and easily reoccur.
Treatment of Phlebolymphedema.
For mild cases of phlebolymphedema, weight loss, leg elevation, exercise, and wearing graduated compression stockings may be sufficient to reduce and control the leg swelling. However, for more significant phlebolymphedema, a more comprehensive treatment program may be required. Possible interventions of an aggressive treatment program may include:
- Manual Lymphatic Drainage massage (MLD). MLD is a very light, specialized massage that stimulates uptake and removal of fluid from the tissue spaces by lymphatic vessels.
- Short-Stretch Compression Bandaging. Short-stretch bandages also called “lymphedema bandages”, are used in combination with padding materials to wrap the swollen legs. The limited stretch of these special compression bandages provides a firm counter-pressure to the muscles of the legs when they contract. This improves compression of veins and lymphatic vessels by the contracting muscles which help to remove the extra fluid from the tissue spaces.
- Exercise. Repetitive muscle contraction improves the efficiency of venous blood flow and lymph transport. Exercise can be done as isolated muscle contractions like ankle pumps, or as ambulation. For individuals without wounds, pool exercise can be beneficial as the pressure on the legs from the water makes muscle contraction more effective.
- Compression Stockings. Once the lymphedema has been reduced, continued compression of the leg will be required to control the re-accumulation of extra fluid. While short-stretch compression bandaging is very effective for initially reducing the lymphedema, graduated compression stockings are usually more practical for long-term, daily maintenance compression. Compression stockings should not be bought at a discount retailer or department store, but rather, they should be provided by an experienced compression stocking fitter.
- Pneumatic Pumps. A pneumatic pump (also known as a compression pump or a lymphedema pump) is an electric pump that inflates multiple air chambers within an inflatable compression garment. The air chambers inflate and deflate sequentially and compress veins to improve venous blood flow, but also direct lymphatic fluid from lymphatic vessels that don’t work to lymphatic vessels that can remove the fluid from the tissues. You should consult your healthcare provider before using any pneumatic pump.
- Endovenous Ablation of Veins that are Not Working Properly. This procedure involves inserting a small laser through a tiny needle stick in the vein. The laser then uses heat energy to collapse the bad veins. The treatment is fast, usually taking only 30-60 minutes to perform, and patients can usually drive and resume light exercise such as walking. immediately. Compression stockings are worn after the procedure for approximately two weeks to promote proper blood flow, comfort, and healing.
Final Words. Phlebolymphedema can be caused by chronic venous insufficiency, problems with lymphatic vessels and lymph nodes, or a combination of both. Being overweight and having a sedentary lifestyle can make phlebolymphedema worse. In addition to the swelling, advanced symptoms of phlebolymphedema can include inflammation, itching, pain, skin fragility, and ulcers, but also thickening of the skin and underlying tissues that reduces blood flow and traps fluid. Patients with phlebolymphedema should seek medical attention and be evaluated for appropriate treatment options to reduce and prevent the progression of the swelling and associated problems.
 507-322-6967
507-322-6967